San Francisco, CA, USA August 22, 2007
Despite the glacial pace of change in healthcare transaction handling, the status quo will gradually give way to a new order.
The current modus operandi in healthcare transaction handling is unsustainable, plagued by the inefficiencies born from highly fragmented stakeholders with conflicting interests and thousands of proprietary formats. Change is a must.
In the second report of its new Healthcare Banking research service, , Celent discusses how some change agents are emerging from the status quo, while newcomers and outsiders are bringing new models. These players will differ notably from their predecessors in that they will enable cooperation across stakeholders and build business models based on aligning costs and benefits. They will reduce the current lack of transaction transparency and improve the current environment of distrust and lack of cooperation. The new order is manifesting itself in various manners, from the operational (e.g., the gradual shift to electronic remittances and ACH) to the organizational (e.g., partnerships spanning the revenue cycle).
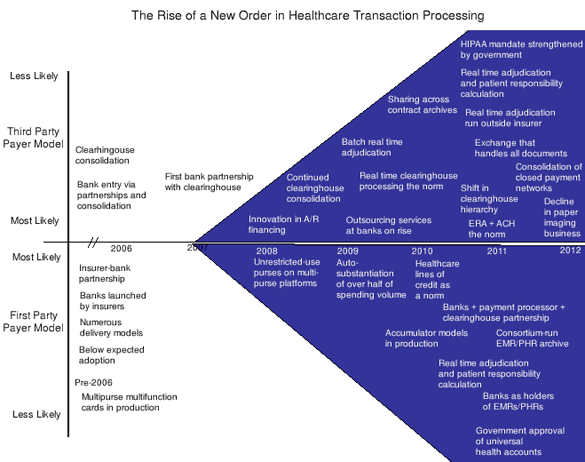
"The third party players, which are showing themselves to be the change agents today, will become leaders. Because they understand the necessity to shift from an infrastructure that handles thousands of payers (third parties) to one that can handle millions of payers (consumers), from an exchange that handles claims and payment documents to one that handles clinical information such as electronic health records and diagnostic results, and from a batch processing platform to a real time one," says Alenka Grealish, coauthor of the report and Managing Director of the Banking team.
Celent estimates that there were around 3.4 billion claims, translating into approximately 1.1 billion payments in 2006. Nearly half (45%) of the 3.4 billion claims were submitted by providers in nonstandard format, while approximately 65% of the remittances were paper. Over the next five years, the use of standard formats and e-remittances will ever so incrementally grow. By 2012, Celent expects that the use of nonstandard claim formats will have dropped to 15%, and the use of e-remittances will rise to 62%, though the use of a common 835 standard is unlikely.
"Among financial institutions, the leaders will be those that facilitate the migration away from paper to electronic and develop innovative receivables financing. Financial institutions must remember that while the number of providers is greater, payers control a larger number of these transactions. Forward-thinking ones must combine their provider-focused extended lockbox offerings with payer-focused solutions that allow paper to be eliminated at its source rather than merely imaged after the fact," comments Madhavi Mantha, coauthor of the report and senior analyst.
The report is 55 pages and contains 21 figures and seven tables (with an additional eight pages, four figures, and two tables of background material contained in an Appendix).
A table of contents is available online. Eight change agents are profiled: athenahealth, the Bank of New York Mellon, InstaMed, MedAvant, MisysPayerpath, Payformance, PNC Bank, and RMS.
Members of Celent's Healthcare Banking research services can download the report electronically by clicking on the icon to the left. Non-members should contact info@celent.com for more information.




